



Challenges to communication in health care
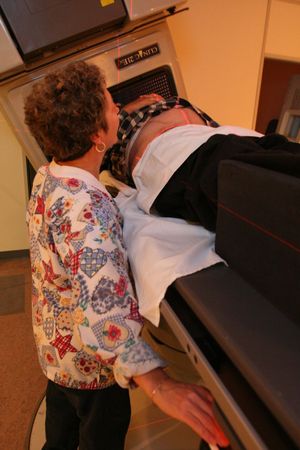
The more specialized the care we provide, the bigger the team and the more complex and important communication becomes.
Health care has become increasingly complex - people in hospital are sicker, the stays are shorter and the team is larger. There is no doubt that advances in surgical care, the medical management of some diseases and care at the extremes of age are great advances. With these advances has come an increased intensity to the work that we do. Interventions and exchanges carry more weight in this world of high acuity, 24/7 care.
"...while specialization of health-care practitioners can improve medical treatment, specialization of care also means more people and units are involved in the patient’s care, which can complicate communication."[1]
The interventional radiologist may not know the referring physician and will not meet the nurse who is caring for the patient overnight after a complicated procedure, but they all depend on one another to complete the circle of care.

Like the blind men and the elephant[4] we all have an understanding of our part of the whole, but only when we put all of our information together can we really complete the picture. Fractured care and providers who do not communicate well place an unnecessary burden on patients and families to provide information or to try to access information that is not available to them.
The traditional hierarchy of health care has changed somewhat but is not gone. Who dares to question the authority of the surgeon?
If we are to work and provide care within a culture of safety then all people involved in the care of the patient must be heard and valued. No one person or provider has the whole picture, or is with the patient the whole time. We need to communicate with one another to provide the seamless care that patients deserve and that is the safest. We need to make space for everyone’s voice to be heard, we need to dampen the hierachy.
Airline pilots have covered this territory before us. Pilots have defined times that they are allowed to work before a period of mandatory rest. Resident physicians are still struggling with the ’duty day’ and how long one can work before safety becomes an issue.[5][6]
Like pilots in the past, medicine has valued autonomy and individual performance. The progression of health-care being provided by a multi-disciplinary team of experts in a variety of fields challenges all providers, but those who have traditionally been the most autonomous might be the most challenged by these changes.[1]
When thinking about hierarchies some people refer to an authority gradient, that is the psychological distance between a supervisor and a worker. Hierarchy can then be defined as the steepness of the authority gradient. [7] Even if we agree with the need for change, it may still be stressful or threatening.
"...the occurrence of everyday medical mishaps is associated with faulty communication; but poor communication is not simply the result of poor transmission or exchange of information. Communication failures are far more complex and relate to hierarchical differences, concerns with upward influence, conflicting roles and role ambiguity, and interpersonal power and conflict." [3]
_________________________________
1. World Health Organization. Communication During Patient Hand-overs. Patient Safety Solutions. 2007;May. Available from: www.ccforpatientsafety.org/Patient-Safety-Solutions/
3. Marshall P, Robson R. Preventing and Managing Conflict: Vital Pieces in the Patient Safety Puzzle. Healthcare Quarterly. 2005;8:39-44.
4. en.wikipedia.org/wiki/Blind_men_and_an_elephant
5. PAIRO - Professional Association of Internes and Residents of Ontario www.pairo.org/Content/Default.aspx?pg=1088
6. Hours Watch www.hourswatch.org/index.htm
7. Wachter RM, Understanding Patient Safety.McGraw-Hill;2008.
 Previous
Previous

