



Burnout and Secondary Traumautic Stress(STS)
Burnout is work-related hopelessness and feelings of inefficiency. Burnout is about being WORN OUT.
Burnout is a commonly used term, for our purposes we consider it to be associated with feelings of hopelessness and difficulties in dealing with work or in doing your job effectively. These negative feelings usually have a gradual onset. They can reflect the feeling that your efforts make no difference, or they can be associated with a very high workload or a non-supportive work environment.
STS is work-related secondary exposure to extremely of traumatically stressful events. STS is about being AFRAID.
Secondary Traumatic Stress is an element of Compassion fatigue and is related to Vicarious Trauma. STS is about your work-related, secondary exposure to extremely stressful events.
Primary trauma is when the event happens to you, such as being a firefighter or front line in a conflict situation as a soldier or humanitarian aid worker.
Secondary trauma is sometimes called vicarious trauma, the trauma that comes from heating stories about traumatic events that have happened to others. Working in emerg or child protections are examples of work where secondary trauma is common.
STS usually comes on quickly and occurs after a specific event. You may feel afraid, have difficulty sleeping, re-experience images of the event unexpectedly or find yourself avoiding things that remind you of the event. If you feel yourself to be more cynical and disconnected from your loved ones that you would like you may be suffering the effects of vicarious trauma.
These two share a negative affect and can often be found together, both are part of compassion fatigue. Burnout is more common and can preceed STS. The frightened, traumatized state of STS is less common but more powerful than good old burnout.
The relationships between these elements are complex. This image might help clarify things:
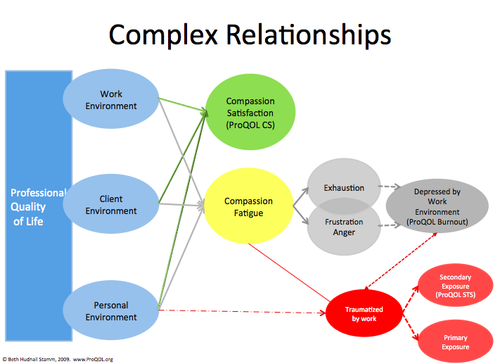
The Professional Quality of Life Scale(ProQol) can measure compassion satisfaction and compassion fatigue. This is not a psychological test or meant to be diagnostic, it is to help you to understand and give name to some of the stresses and satisfactions you may be experiencing. If anything, it can be considered a screening test for health problems. [3]
Low Impact Debriefing
Françoise Mathieu is a Compassion Fatigue Specialist based in Kingston. Her paper "Running on Empty: Compassion Fatigue in Health Professionals" is an excellent and practical introduction to the topic and is available on her website at this link. You may have had the good fortune of attending a seminar with her, in which case you are aware of compassion fatigue. If you are interested in hearing her speak you can watch a video of her presentation to a group of professionals working in harm reduction. It runs about 90 minutes, but it is a great investment of your time.
In this talk she introduces the concept of ’sliming’ - those times when we are so full of stories that we just empty them onto someone else. While this at first pass may feel beneficial - the act of talking openly and honestly to someone else about the things that effect us at work, the act of bearing witness to the pain and suffering of those we seek to care for. We might actually be inflicting a degree of vicarious trauma on those who provide the listening ear.
Matthieu provides an approach to what she calls ’low impact debriefing’ (available as a PDF from her website compassionfatigue.ca) in which she differentiates between the immediate informal debriefing that we all do on the fly and the formal debriefing that often occurs long after the immediacy of the event in question has passed.
Start with an awareness of how and when you debrief
How much detail do you share when you debrief, at what point are those details vicariously traumatizing to someone else? How essential are they to the story? How central are they to you being able to talk about how the event/story affected you?
Let your listener know that there is a difficult story that you would like to tell.
Ask permission before you unburden yourself - get informed consent! Perhaps your listener is unable to hear such a story right now - it might be the content or the timing of hearing a difficult story. There is then the opportunity to negotiate a different time to talk about it, or to tell a less detailed version of the story that will still meet your needs but not push your listener beyond what they are safely able to hear at that time.
Even being more aware of the power of the stories we carry and how our need to share them can effect others can decrease the impact of our debriefing.
_________________________________
3. Content in this section from the ProQoL website: www.proqol.org www.proqol.org/uploads/proqol_org_helper_pocket_card.pdf
 Previous
Previous