



Introduction to the Oncology Team

Cancer can happen to anyone, at any age, in any body system. It occurs in all geographic regions, races, classes and cultures.
The oncology team diagnose and provide care to the incredibly diverse group of people with cancer. The team for each person will be different, based on need, and availability of services and may change over time. The patients’ needs determine the composition of the team - the patient is at the centre of cancer care team.
Members of the team have:
specialized training, skills and knowledge representing current best-practices and on a strong evidence base
communication skills to meet the educational and emotional needs of patients
a connection with a wider professional group that ensures ongoing education, standards of practice and accreditation
clearly defined skill sets and scopes of practice
Objectives
After completing this module you will be able to:
describe the team approach to cancer care
identify the members of the oncology care team
explain the contribution of each member of the team to the care of patients with cancer
compare and contrast the different approaches to the person with cancer represented on the oncology team
identify the ways in which a multi faceted approach to cancer care benefits the patient, family and care team
describe the oncology team for a specific patient
In this module we will first look at health professions and teams of healthcare professionals and then look at some members of the oncology team, their roles, areas of expertise and ways of working with others to provide care for people with cancer.
Healthcare professionals
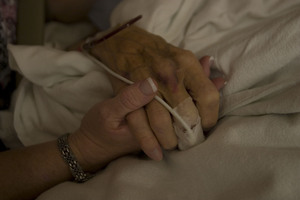
It is the expectation of patients, families and other healthcare providers that we all behave professionally.
We are all professional in our delivery of health care. Some roles are considered to be regulated health professions.
In Ontario there are 21 regulated health professions, each is governed by an independent college that sets standards for knowledge, skills and behaviour for their members. The legal framework for this structure is administered for the provincial government through the Ministry and Long-term Care. The colleges are responsible for the self-regulated functions of the professions as outlined in the Regulated Health Professions Act.
Healthcare teams working for patients

Working together
Many professions and professional bodies have addressed the need to learn together, to know about one another and to work together in codes of ethics, standards of practice and descriptions of roles, a few examples of these are listed below:
Discipline | Document | Reference |
Nursing | Code of Ethics | Health and Well-being, 7. In providing care, nurses should also respect and value the knowledge and perspectives of other providers. They should actively collaborate and where possible seek appropriate consultations and referrals to other health team members in order to maximize health benefits to people. Quality Practice Environments, 10. Nurses should collaborate with nursing colleagues and other members of the health team to advocate for health care environments conducive to ethical practice and to the health and well-being of clients in the setting. They do this in ways that are consistent with their professional role and responsibilities.[1] |
Medicine |
CMA code of ethics
| 47. Be willing to teach and learn from medical students, residents, other colleagues and other health professionals. 52. Collaborate with other physicians and health professionals in the care of patients and the functioning and improvement of health services. Treat your colleagues with dignity and as persons worthy of respect.[2] |
| Royal College of Physicians and Surgeons of Canada - CanMEDS Roles - Collaborator
| As Collaborators, physicians work within a healthcare team to achieve optimal patient care. Physicians work in partnership with others who are appropriately involved in the care of individuals or specific groups of patients. This is increasingly important in a modern multiprofessional environment, where the goal of patient-centred care is widely shared. Modern healthcare teams not only include a group of professionals working closely together at one site, such as a ward team, but also extended teams with a variety of perspectives and skills, in multiple locations. It is therefore essential for physicians to be able to collaborate effectively with patients, families, and an interprofessional team of expert health professionals for the provision of optimal care, education and scholarship. Key competencies: 1. participate effectively and appropriately in an interprofessional healthcare team. 2. Effectively work with other health professionals to prevent, negotiate, and resolve interprofessional conflict.[3] |
Dietitians | Canadian Oncology Nutrition Standards of Practice | Section I, Standard 4 - Membership in Interdisciplinary Teams. Oncology dietitians are members of oncology interdisciplinary health care teams. Section II, Standard 21 - Continuity of Care. Oncology dietitians work in partnership with health care and community resources to provide continuity of nutrition services for clients and their families across the cancer continuum. Standard 24 - Health Care Team Members.Oncology dietitians: a. provide oncology nutrition knowledge and expertise to the health care team. b. incorporate the role of nutrition services into the care pathways of relevant tumour site teams. c. advocate for the provision of nutrition services within comprehensive cancer care. d. act as client advocates. "[CONSoP |
Health Canada
| Interprofessional Education for Collaborative Patient-Centred Practice | Collaborative patient-centered practice is designed to promote the active participation of several health care disciplines and professions. It enhances patient-, family-, and community-centred goals and values, provides mechanisms for continuous communication among health care providers, optimizes staff participation in clinical decision making (within and across disciplines), and fosters respect for the contributions of all providers. There is growing consensus that interprofessional collaborative patient-centered practice - across all health sectors and along the continuum of care - will contribute to the following: improved population health / patient care;improved access to health care;improved recruitment and retention of health care providers;improved patient safety and communication among health care providers;more efficient and effective employment of health human resources; andimproved satisfaction among patients and health care providers."[4] |
For an introduction Interprofessional Education, see the companion module to this one and learn about "learning together to work together".
_________________________________
1. Code of Ethics for Registered Nurses, Canadian Nurses Association, August 2002 ISBN 1-55119-890-8 http://www.cna-aiic.ca/CNA/practice/ethics/code/default_e.aspx accessed February 5, 2008
2. CMA Code of Ethics, 2004. Canadian Medical Association. http://www.cma.ca accessed February 5, 2008
3. The CanMEDS 2005 Physician Competency Framework, The Royal College of Physicians and Surgeons of Canada. http://rcpsc.medical.org/canmeds/CanMEDS2005/index.php accessed February 5, 2008.
4. Health Canada.Interprofessional Education for Collaborative Patient-Centred Practice. http://www.hc-sc.gc.ca/hcs-sss/hhr-rhs/strateg/interprof/index_e.html accessed February 5, 2008.
